Raise Engagement, Simplify Compliance
PDHI’s Wellness Platform for health plans helps you deliver configurable programs that identify health risks, promote and reward gaps-in-care closure, and drive sustainable behavior change to meet critical quality measures.

Integrated + Holistic Population
Health Management
Our platform helps you deliver configurable programs that seamlessly meet critical quality measures, helping you identify health risks, promote and reward gaps-in-care closure, and drive sustainable behavior change.
Flexible
Integration
White-label platform adapts to your needs and seamlessly integrates with your member portal.
Engage, Motivate, Challenge
Engage participants through effective health appraisals, self-management tools, and incentive programs.
Industry-leading Compliance
Whether used as integrated modules or a complete solution, PDHI helps you meet industry regulatory compliance and security standards.
Solutions to Meet All Your Needs
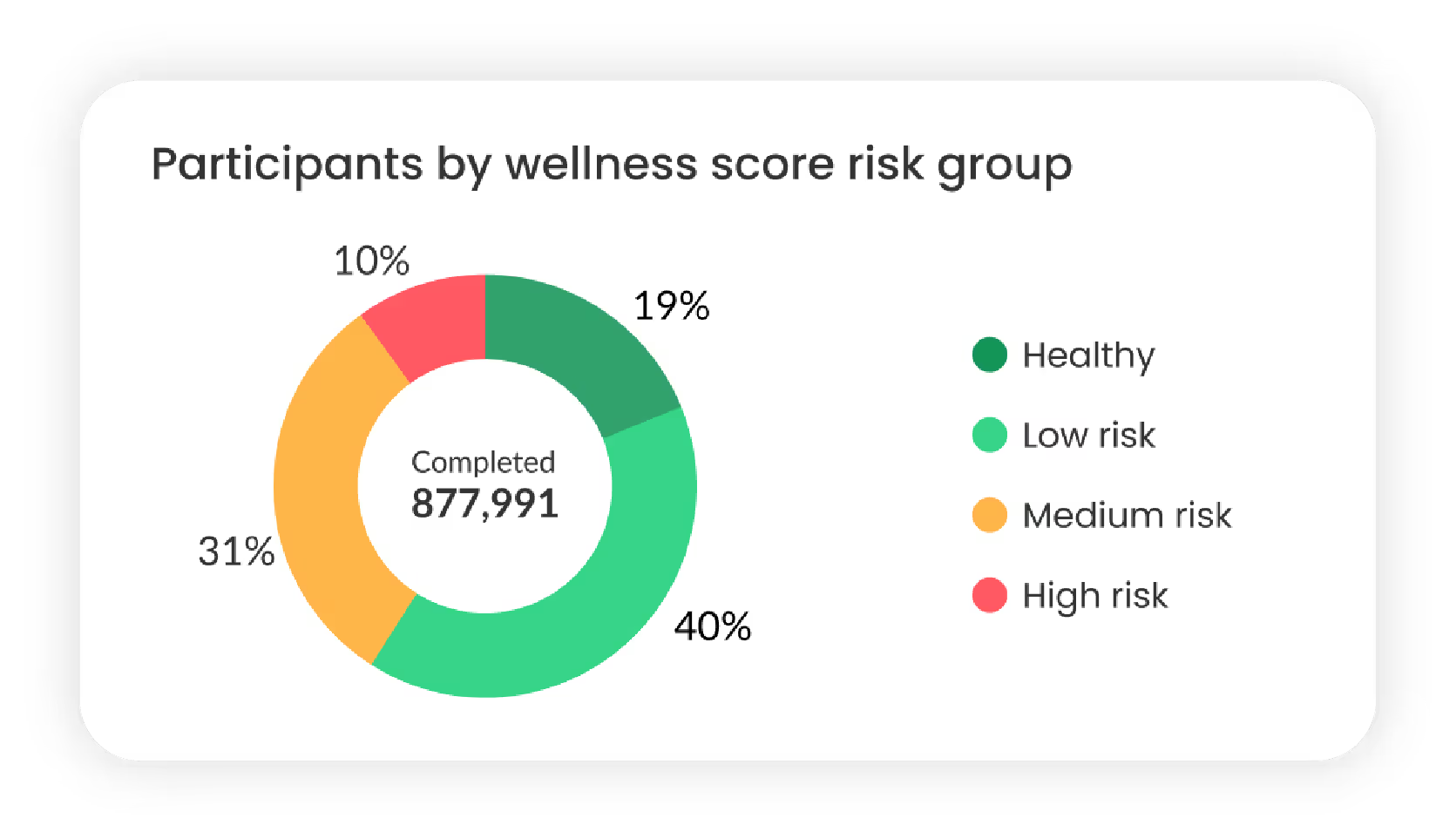
Managed Health Assessments
Fulfill state and federal health assessment requirements for new enrollees and existing plan members using digital tools and tech-enabled services. NCQA-certified and custom health assessments can address your needs across diverse populations.

NCQA Compliance
Receive automatic credit for your NCQA Health Plan Accreditation with our solutions, avoiding high costs of building and maintaining on your own. Deploy NCQA-certified health appraisals and self-management tools — directly embedded in your member portal.
Incentives Management
Incentivize members to complete healthy actions using tailored reward programs that motivate behavior change, close gaps in care, and improve outcomes.
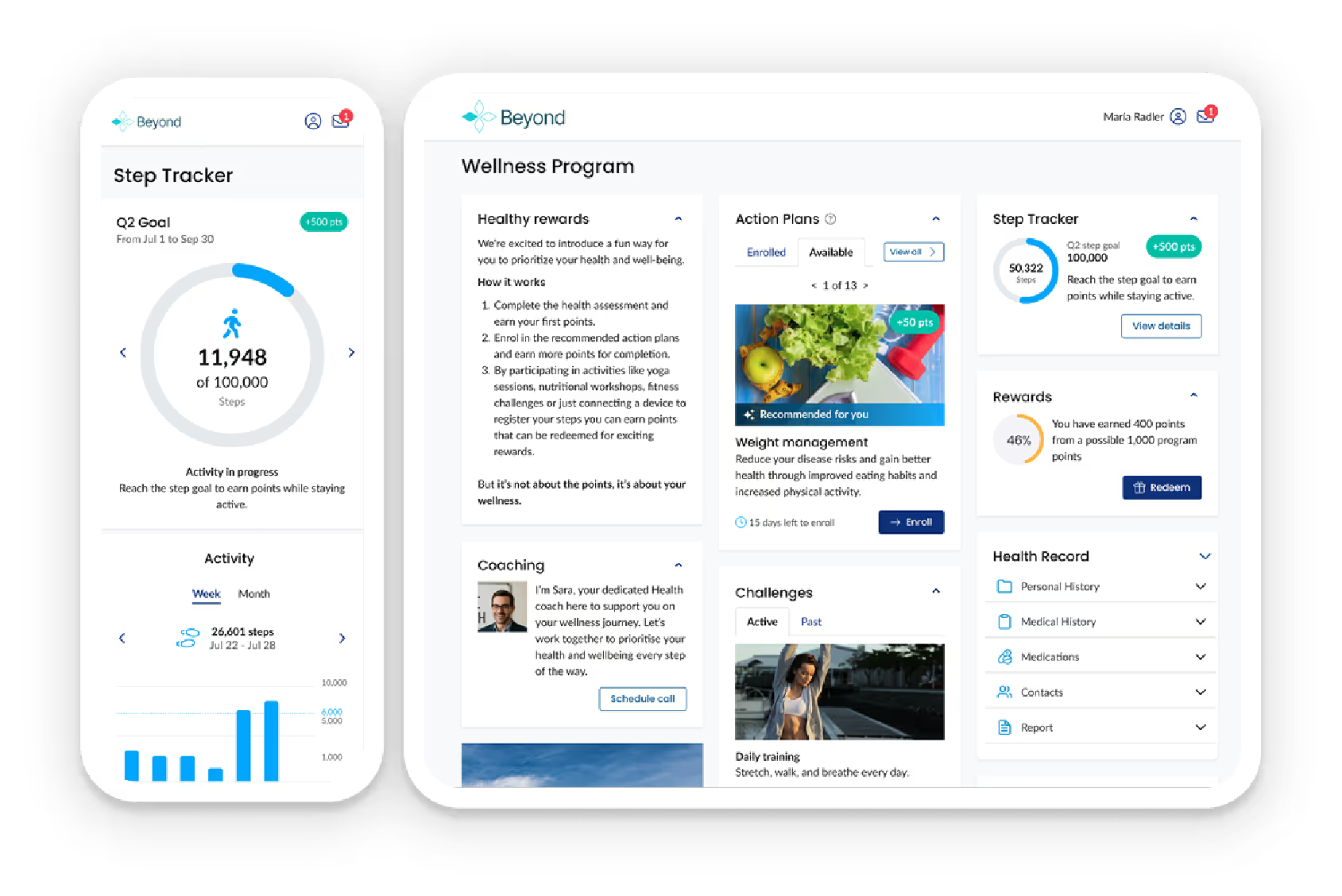
Member Engagement + Wellness Platform
Encourage members along their health journey with a proven set of digital wellness tools that identify health risks, promote healthy behavior change, and track progress towards health goals.
Your Partner in Deployment
Our SaaS platform was built to support scale and security, allowing you to focus on building the best programs for your employees’ needs.
Employer groups supported
Average time to implementation
Supporting population health and wellness initiatives
See Our Solutions in Action
Simplify Regulatory Compliance
See how one Medicare Advantage plan received auto-credit during their NCQA accreditation process by using PDHI's certified health appraisal.
Close Gaps in Care
A California Medicaid plan improved internal outreach and care management using the data collected with the ConXus Platform, resulting in fewer care gaps.
Meet Quality Initiatives
See how a Midwestern health plan uses PDHI to streamline wellness and population health, close care gaps, and deliver assessments for 350,000 members—driving quality initiatives for over 15 years.
Engage + Retain Members
A Northern Health Plan upgraded its health assessment process for its 300,000 Medicaid, Medicare, and commercial members to engage its members using the ConXus Platform.
Can the platform handle multiple lines of business under one administration layer?
Yes. Configure distinct experiences by line of business — Medicare Advantage, Medicaid, commercial — while managing eligibility, incentives, and reporting from a single admin layer.
How does PDHI support quality improvement and gap closure?
The PDHI Health Assessment is a certified HRA that supports NCQA accreditation, including auto-credit recognition, and feeds care management workflows to close gaps in care.
Can the platform scale to large member populations?
Yes — one Midwestern health plan has used the PDHI Platform to serve more than 350,000 members for over 15 years.
Can member experiences be personalized by population segment?
Yes. The platform supports multi-population segmentation, so you can deliver targeted programs, communications, and incentives based on health risk, plan type, or member demographics.
What reporting is available for plan leadership and stakeholders?
Administrators have access to real-time program insights and in-depth reports on participation, engagement, and outcomes — exportable to external systems or data warehouses.
Ready to Elevate Your Member Engagement Strategy?
From closing care gaps to meeting compliance requirements to improving member satisfaction— let's explore how our flexible, proven solutions can support your goals.

